Peer To Peer Review Prior Authorization

Peer To Peer Review Process Discontinued

Form Fa 70a Download Fillable Pdf Or Fill Online Prior Authorization Request Psychotropic Agents For Children Age 0 To 5 Nevada Templateroller

How To Deal With Prior Authorization Hassles In The Wound Clinic Today S Wound Clinic

Authorization Coordinator Resume Samples Qwikresume
2
2
Peer to Peer Requirements Prior to issuing a medical necessity denial in response to an authorization request for medical or pharmacy services, a representative calls the treating provider and offers to schedule a peertopeer review The review should take place prior to issuance of the denial Scott and White Health Plan (SWHP) requests providers to promptly respond to the peer to peer request in order to ensure a timely and effective review of authorization requests for medical services.

Peer to peer review prior authorization. If you are requesting a Tier II or NonPreferred antipsychotic drug for any child within the 10 to 17 year age range, the Tier II and NonPreferred prior authorization will ONLY be approved for a LIMITED TIME The child will then need to be converted into the peer review program Based on the schedule below, you will be contacted by someone from the Peer Review Program. Prior authorization is a "condition of payment" and is required for the listed OPD codes by CMS If a PAR is not obtained, the denied claim may be appealed, however these services will not subject to additional review. A PeertoPeer Review or Reconsideration can be requested for prior authorizations that are denied or modified If you request a PeertoPeer and afterward determine a Reconsideration is appropriate, the.
Evolent Health (Evolent) is managing all level one appeals and peertopeer reviews for Premera Blue Cross (Premera) Individual Plan members Premera will handle level two appeals To submit a clinical appeal on behalf of a patient (denied prior authorization), do one of the following Submit an appeal form by fax to The new appeal form will be on the provider secure site and the Premera nonsecure website under “Forms” starting January 1,. Prior authorization (PA) to be reviewed if the determination is denied or reduced The two options are a peertopeer review or reconsideration PeertoPeer Review Before submitting a written request for reconsideration, the requesting provider may request a peertopeer review. What is a peer to peer prior authorization?.
Take advantage of a payer’s peertopeer process Speaking to the insurer’s medical director or other physician available to speak with physicians about prior authorization issues can clear up. 2 Complete Section III if this request requires a peer to peer review 3 Complete Section IV if this request is a renewal 4 Prescriber Sign and date the form prior to submission SECTION I MEDICATION REQUESTED Select the appropriate medication(s) for this request. Prospective review This is the prior authorization or precertification process conducted at the onset of a treatment or service The review is performed before the service is provided so as to eliminate or minimize medically unnecessary services Concurrent review This review is performed in the course of treatment or episode of care.
1 You can ask for one PeertoPeer Review The treating provider can request a PeertoPeer Review with the physician reviewer within 5 calendar days of the date on the authorization denial letter To make the request Call Molina Healthcare Utilization Management at (855) or Advance Imaging at. July 24, Prior authorization denials are an infuriating headache for practices, especially when they result in a peertopeer review—placing an administrative stranglehold on clinical operations & busy surgeons Providers spend hours gathering documentation for submission only to have the prior authorization denied by the payer. The prior authorization shall not be denied if the subscriber has a terminal illness on behalf of the covered person a peertopeer conversation regarding an adverse request peertopeer review Plan must establish a review process at which the covered person has.
Electronic prior authorization software is available to ease the work load and increase the efficiency of obtaining prior auths On average, practices who’s primary method of obtaining precertification, report a 94% reduction in workload, and a 50% reduction in cost––money that certainly be put to better use elsewhere. In addition, both peertopeer review call and prior authorization are required to obtain approval for hyperbaric oxygen therapy (HBOT), negative pressure wound therapy (NPWT), and cellular and tissuebased products (CTPs). The Power of a PeertoPeer Identifying an Unrecognized Clinical Condition Sometimes a request for care—no matter how wellintentioned— is denied during the prior authorization process When this happens, providers can learn more about the decision, and in certain circumstances have it reevaluated, by speaking with an eviCore clinician.
Prior Authorization Process •Determinations to deny or reduce the request for authorization results in written notification to the member and provider of the decision, rationale for the decision, the criteria or guideline applied and not met, and the appeal rights. To peer review of a determination on either an inpatient or outpatient authorization request is to exchange information about the clinical nuances of the member’s medical condition and the medical necessity of the services. Assists medical staff and Patient Access RN in all aspects of the PeertoPeer Review Program, financial clearance, and medical necessity check Communicates with clinical counterparts at the payer and within the cancer center Organizes and prioritizes encounters needing financial clearance due to pending peertopeer reviews.
Request a peertopeer The phone number to request a peertopeer is Providers have up to 5 calendar days after the issuance of the denial to request a peertopeer The phone number to request a peertopeer is Inpatient Providers have up until the date of discharge to request a peertopeer For all other services. Effective April 1, , the Inpatient Hospital Review Program (IHRP) was suspended due to the Public Health Emergency related to COVID19 pandemic Inpatient claims in which the admit date occurs on or after April 1, , will not require an IHRP prior authorization, concurrent or complex case review during the Public Health Emergency (PHE) PARs still need to be entered for Transplants and Out of State inpatient admissions. We know the peertopeer process sometimes can be a challenge That’s why we are making online scheduling faster for you and your staff To help simplify the scheduling process, we’ve updated our PeertoPeer Scheduling Request form with the ability to submit it directly from the website.
Prior authorization is often required by insurance companies for services such as MRI’s, PET scans and many prescription medications When a prior authorization is requested it means that the insurance carrier needs more information before making a final decision on whether it will be covered. PeertoPeer Conversation PrimeWest Health professionals who conduct clinical review of Service Authorization requests are available to discuss review determinations with attending physicians or other ordering providers This review can occur by telephone, in person, or by secure email. Assists medical staff and Patient Access RN in all aspects of the PeertoPeer Review Program, financial clearance, and medical necessity check Communicates with clinical counterparts at the payer and within the cancer center Organizes and prioritizes encounters needing financial clearance due to pending peertopeer reviews.
Peertopeer review is a process in which an ordering physician discusses the need for a procedure or drug with another physician who works for the payer in order to obtain a PA approval or appeal a previously denied PA. Prior authorization (PA), to ensure that they are medically necessary and appropriate for the reason prescribed before they can be covered PAs help manage costs, control misuse, and protect patient safety, as well as ensure the best possible therapeutic outcomes. Medicaid Providers Updated Prior Authorization Tips and PeertoPeer Discussion Process (One Change Effective May 1, 21) days of the adverse determination and the fax cover sheet must be clearly identified as the wish for a clinical rereview in lieu of a peertopeer discussion If an appeal has been filed during this period, the peer.
Peer to Peer Scheduling Request Form UnitedHealthcare offers the opportunity for your physician to speak with our medical director to discuss the medical policy and documentation requirements which determined the response for your prior authorization or concurrent review request. Prior authorization — also frequently referred to as preauthorization — is a utilization management practice used by health insurance companies that requires certain procedures, tests and medications prescribed by healthcare clinicians to first be evaluated to assess the medical necessity and costofcare ramifications before they are authorized. To meet this goal, the program has established a prior authorization (PA) process As always, a PREFERRED antipsychotic (see Preferred Drug List at http//wwwprovidersynergiescom/services/documents/MDM_PDLpdf) does not require a prior authorization, if prescribed within the FDA Guidelines for the dose and frequency Clinical criteria have been established which must be met before a Tier 2 & Nonpreferred (Tier 2 & NP) antipsychotic is approved.
Peertopeer review is a process in which an ordering physician discusses the need for a procedure or drug with another physician who works for the payer in order to obtain a PA approval or appeal a previously denied PA. What is a peer to peer prior authorization?. Not to be confused with a medical peer review, this is solely something that happens when a request for services has been denied by the insurance company This can also be called a "doc to doc" appeal, this is typically a phone conversation between a physician at an insurance company (the one that's refusing to pay for services) and the patient.
Prior authorization denials are an infuriating headache for practices, especially when they result in a peertopeer review — placing an administrative stranglehold on clinical operations and busy surgeons Providers spend hours gathering documentation for submission only to have the prior authorization denied by the payer. We encourage you to call the Prior Authorization department at for all urgent requests Peer to Peer Consultations Peer to peers are scheduled by calling ext 1 within the timeframe outlined in the denial notification. In the peertopeer consultation, Peer 1 — that sounds too much like a store, so let’s say Peer A — the insurance company physician, almost never trained in oncology and Peer B (me) discuss, by phone, the medical scenario of the patient and why she is in need of the previously denied, prescribed service.
Not to be confused with a medical peer review, this is solely something that happens when a request for services has been denied by the insurance company This can also be called a "doc to doc" appeal, this is typically a phone conversation between a physician at an insurance company (the one that's refusing to pay for services) and the patient. Peertopeer review is a process in which an ordering physician discusses the need for a procedure or drug with another physician who works for the payer in order to obtain a PA approval or appeal a previously denied PA If properly implemented, the process can be helpful, as it affords the physician the opportunity to speak with another clinician. Request a peertopeer The phone number to request a peertopeer is Providers have up to 5 calendar days after the issuance of the denial to request a peertopeer The phone number to request a peertopeer is Inpatient Providers have up until the date of discharge to request a peertopeer For all other services.
Take advantage of a payer’s peertopeer process Speaking to the insurer’s medical director or other physician available to speak with physicians about prior authorization issues can clear up. Before beginning the reconsideration and appeals process, treating providers can request a PeertoPeer discussion with a doctor to review details of the member’s condition and care options Expedited Appeals are available for members who are at a more urgent risk for severe health issues without the previously requested care or service. Effective April 1, , the Inpatient Hospital Review Program (IHRP) was suspended due to the Public Health Emergency related to COVID19 pandemic Inpatient claims in which the admit date occurs on or after April 1, , will not require an IHRP prior authorization, concurrent or complex case review during the Public Health Emergency (PHE) PARs still need to be entered for Transplants and Out of State inpatient admissions.
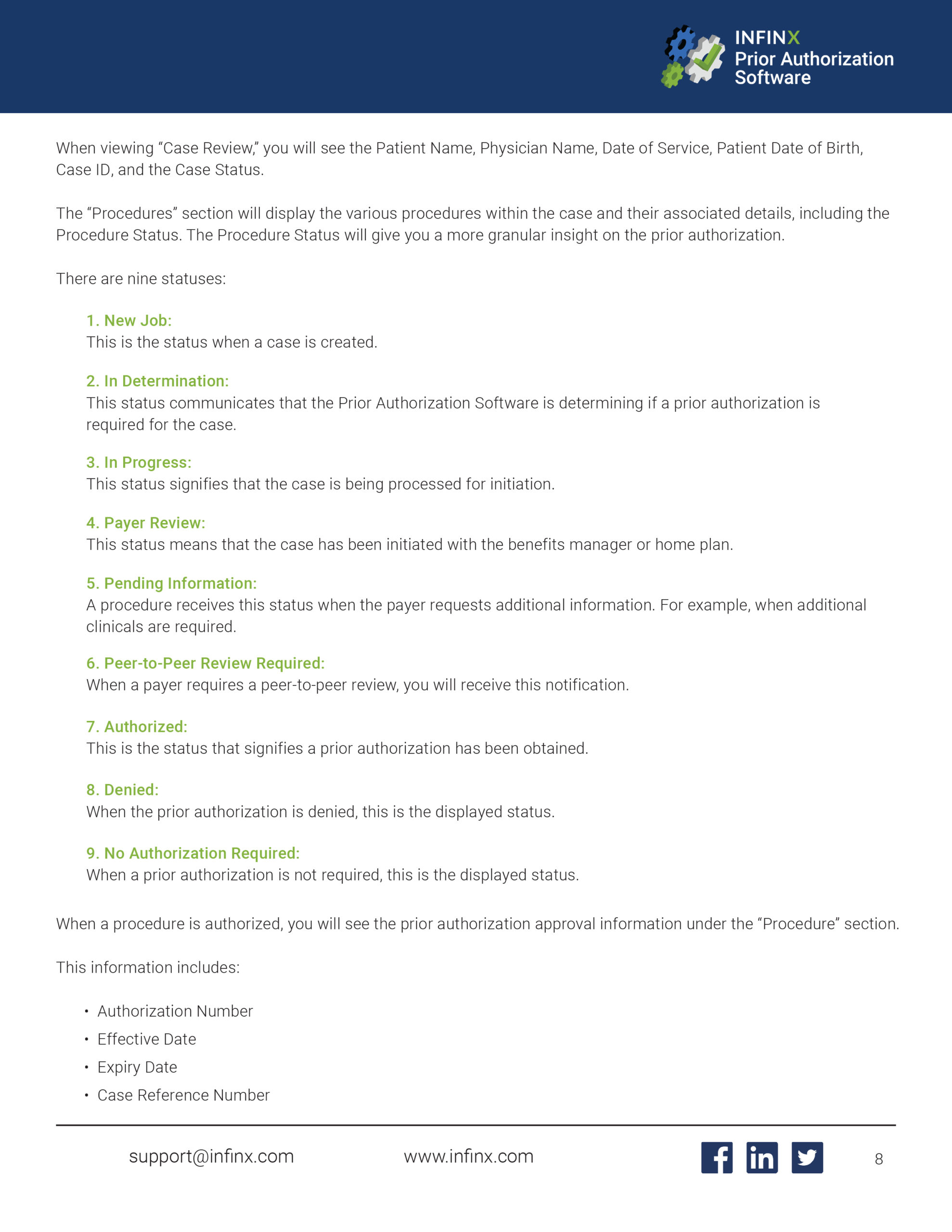
Prior Authorization determines whether an authorization is required and automates data retrieval from payer websites, capturing screenshots status Prior Authorization verifies requirements and automates logging in to payer portals, autopopulating data to complete an authorization request up until clinical data is required. Peertopeer review is a process in which an ordering physician discusses the need for a procedure or drug with another physician who works for the payer in order to obtain a PA approval or appeal a previously denied PA. What is a peer to peer prior authorization?.
A prescriber can submit a Prior Authorization Form to Navitus via US Mail or fax, or they can contact our call center to speak to a Prior Authorization Specialist The request processes as quickly as possible once all required information is together. Before beginning the reconsideration and appeals process, treating providers can request a PeertoPeer discussion with a doctor to review details of the member’s condition and care options Expedited Appeals are available for members who are at a more urgent risk for severe health issues without the previously requested care or service. Peer to Peer Requirements Prior to issuing a medical necessity denial in response to an authorization request for medical or pharmacy services, a representative calls the treating provider and offers to schedule a peertopeer review The review should take place prior to issuance of the denial.

Montana Medicaid Drug Prior Authorization Program Outpatient Drug
Fm Formularynavigator Com Formularynavigator Documentmanager Download Clientdocumentid Pchmwfk Z0qnmthpkayucw

8 Prior Authorization Terms That Drive Every Doctor Crazy American Medical Association
Tuftshealthplan Com Documents Providers Forms Medication Request Form
Stories Fix Prior Auth
Ipa Release Notes 4 0 Aug Infinx

Pros And Cons Of Prior Authorization For Value Based Contracting
Www Regrelief Org Wp Content Uploads 19 12 Rrc Prior Authorization Survey Results Final 7 26 Pdf
Q Tbn And9gcqxiqtg60fzqttqyrtwkubz2awljbhilwuh86jljhmyppjbttb1 Usqp Cau
Www Fideliscare Org Portals 0 Providers Educationalmaterials 19 Fideliscare Niaphysicalmedicineproviderfaq English Pdf
Beonbrand Getbynder Com M 6a5c2b8eb9db705e Original Radiology Program Faq Pdf
2

How To Deal With Prior Authorization Hassles In The Wound Clinic Today S Wound Clinic

How Ai Is Cutting Prior Auth Denials Reducing Peer To Peer Reviews Verata Health

Pdf Technology Enhanced Peer Review Benefits And Implications Of Providing Multiple Reviews

Form Fa 162 Download Printable Pdf Or Fill Online Protopic Tacrolimus Prior Authorization Request Form Nevada Templateroller

Streamlining And Reimagining Prior Authorization Under Value Based Contracts A Call To Action From The Value In Healthcare Initiative S Prior Authorization Learning Collaborative Circulation Cardiovascular Quality And Outcomes
Www Molinahealthcare Com Providers Wa Medicaid Comm Pdf Peer To Peer Changes Pdf

Wyoming Equalitycare Policy For Wyoming Medicaid

Vcax5nn Fcskem

Priorityhealth Prior Prescription Rx Authorization Form Authorization Forms
2

Peer To Peer Utilization Review Modern Meded
Dfs Ny Gov System Files Documents 01 Ul Min Prior Req Pdf

Kadcyla Avmed

ns Neurosurgeon Prior Authorization The Filibuster Of Healthcare ns Neurosurgeon

8 Prior Authorization Terms That Drive Every Doctor Crazy American Medical Association

Medication Access Report Covermymeds

A Look Into Peer To Peer Blog Prior Authorization Training

Peer To Peer Review Process Discontinued
:max_bytes(150000):strip_icc()/mature-man-in-wheelchair-with-doctor-and-nurse-578202471-5a26bd66e258f8003b5615ec-4ea8e5e5ff02411195e511d0bb0e9823.jpg)
How To Get A Prior Authorization Request Approved
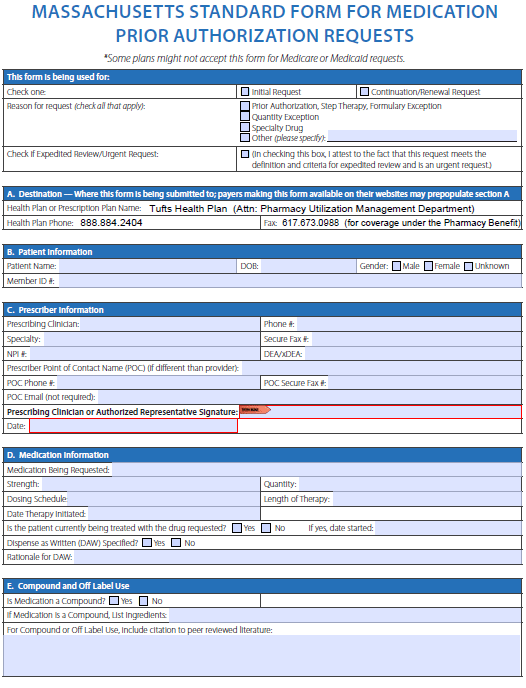
Tufts Prior Prescription Rx Authorization Form Authorization Forms

Prior Authorization As A Utilization Management Tool For Elective Superficial Venous Procedures Results In High Administrative Cost And Low Efficacy In Reducing Utilization Journal Of Vascular Surgery Venous And Lymphatic Disorders

Prior Authorization Washington State Local Health Insurance Chpw

The Ultimate Guide To Prior Authorization Myndshft
Www Ecommunity Com Sites Default Files Uploads 19 03 Health Direct News Mar19 Pdf

Jakafi Avmed
2
2

Frequently Asked Questions

Utilization Management Eqhealth Services
Fm Formularynavigator Com Formularynavigator Documentmanager Download Clientdocumentid Qvmakaegtuywy7p1v7rshw

Beating The Prior Authorization Blues Fpm
Q Tbn And9gcqlyqiuuci3hbotudgq4ieb2tskxja37mt9plykanj2op1tc8bx Usqp Cau
Www Molinamarketplace Com Marketplace Oh En Us Providers Media Molina Publicwebsite Pdf Providers Oh Medicaid Forms Medicaid And Marketplace Guide Pdf

Medication Access Report Covermymeds
Www Aicpa Org Research Standards Peerreview Downloadabledocuments Peerreviewstandardsinterpretations Pdf

Avoid Pre Authorization Pitfalls Following A Few Documentation Guidelines Can Help Speed Approval Of Your Patients Treatment The Asha Leader Vol 23 No 6
/prescription-56a68fa63df78cf7728eff7e.jpg)
How Prior Authorization Works
Q Tbn And9gcsqwwaqo2dl7cqa5zuiqcyniui76taienzvyr8rqxuckmw0oozl Usqp Cau

National Imaging Associates Inc Nia Medical Specialty Solutions Ppt Download

Prior Authorization And Notification Uhcprovider Com

How Ai Is Cutting Prior Auth Denials Reducing Peer To Peer Reviews Verata Health

Fresh Medical Mutual Prior Authorization Form Models Form Ideas

Prior Authorization Of Physical Therapy Occupational Therapy For Wellcare Provider Orientation Thank You For Joining My Name Is I Am With Evicore Ppt Download

Chapter 7 Peer Reviews Using Peer Exchanges To Improve The Effectiveness Of Strategic Highway Safety Plans The National Academies Press
2
2

Form Fa 63 Download Fillable Pdf Or Fill Online Prior Authorization Request Pdl Exception Non Preferred Drugs Nevada Templateroller

Free Envisionrx Prior Rx Authorization Form Pdf Eforms
F Hubspotusercontent00 Net Hubfs peer reviewer application Peer Reviewer Application Pdf

How Prior Authorizations Hurt Patients Diagnosis Life Llc
Content Highmarkprc Com Files Region Pa Newsletternotices Specialbulletins Sb Pa Ma Peer To Peer Process Pdf
Www1 Radmd Com Media Home State Post Service Therapy Faq Pdf
Fm Formularynavigator Com Formularynavigator Documentmanager Download Clientdocumentid Xlyievdnfuyz4 Gisfbinw
Www ns Org Media Files ns Letters ns Cns Statement For The Record Small Business Committee Utilization Review Hearing Ashx La En Hash C0752c02ec50e23decdebca16b7693b235

Become A Peer Reviewer Clinical Advisor
2
2

Oxycodone Controlled Release Medication
Www Huskyhealthct Org Providers Provider Postings Pa Of Genetic Testing Services Pdf

How Ai Is Cutting Prior Auth Denials Reducing Peer To Peer Reviews Verata Health

Ky4vxscvbvcdkm

8 Prior Authorization Terms That Drive Every Doctor Crazy American Medical Association
Q Tbn And9gcsqwwaqo2dl7cqa5zuiqcyniui76taienzvyr8rqxuckmw0oozl Usqp Cau

Anthem Medical Non Oncology Specialty Drug Review Changes
Automated Prior Authorization Catches On Onclive
Www Cloverhealth Com Filer File 966

Impact Of Sequential Opioid Dose Reduction Interventions In A State Medicaid Program Between 02 And 17 The Journal Of Pain

My Access 360 Forms And Resources

A Look Into Peer To Peer Blog Prior Authorization Training

How To Avoid Peer To Peer Phone Calls

Health Insurance Prior Authorization Requirements Its Impact And Recommendations By Mos Medical Reviews Issuu
2

How To Obtain Prior Authorizations Jdrf

How Ai Is Cutting Prior Auth Denials Reducing Peer To Peer Reviews Verata Health

Free North Carolina Medicaid Prior Authorization Form Pdf Eforms
Www1 Radmd Com Media Nhhf Physical Medicine Provider Faq Final Pdf

The Ultimate Guide To Prior Authorization Myndshft
2

Humana Taps Cohere Health To Modernize Prior Authorizations For Musculoskeletal Treatment
2
2

Medication Access Report Covermymeds
2

Authorization Coordinator Resume Samples Qwikresume
Fm Formularynavigator Com Formularynavigator Documentmanager Download Clientdocumentid Udirrlveoesol6ffjdxu Q
Www Uhcprovider Com Content Dam Provider Docs Public Health Plans Oxford Navigating Voice Portal Quick Reference Pdf



